
Fear. Panic. Helplessness. Those are the feelings that swept over me as I lifted my daughter up from the toilet seat. There’s so much blood. I cleaned her up and washed my hands. I grabbed my cell phone, took a photo of the bowl (really), and sent it to Todd. He helped calm and ground me and explained that it was probably nothing to worry about but to call and make an appointment with her doctor. I called and left a message with his office and then contacted Dr. Google. I was reassured by Dr. Google that the bright red color was a good sign, but there were questions about pain levels. I cried because I had no idea if Emily was in pain.
The nurse returned my calls later in the day and said there weren’t any appointments available in our medical group and that I had to take Emily to Urgent Care. My heart sank, and I felt anxiety creep in. The severity of her cognitive delays makes any appointment challenging, but going to an Urgent Care is next level. I knew I had to put on my big girl combat boots and do what needed to be done. I packed everything I thought we might need for a long wait at Urgent Care and drove in silence to pick Emily up from AbilityFirst. I needed a few moments to process my feelings and reframe my thoughts about the situation. I can kick and scream my way through the next few hours or proceed from a place of acceptance. I decided the latter would serve not only me but Emily best.
We entered the Urgent Care, and to my surprise, the waiting area was empty. We arrived during lunch and we had to wait a bit, but we were first in the queue. This gave me peace of mind because Emily was not thrilled about our destination and was letting the staff know–loudly. The nurse called us in. He tried repeatedly to get Emily’s blood pressure. I asked him to stop because it seemed to be upsetting her. (I know how uncomfortable it is when the damn blood pressure machine doesn’t get a read.) He tried one more time and then conceded. He asked about pain levels, which I could not answer. He finally got her heart rate to register. It was elevated.
The nurse practitioner did a quick check for anemia and performed a physical exam, and could not conclude the cause of the blood in the stool. She was concerned about the elevated heart rate and that she was unable (after several more attempts) to get Emily’s blood pressure. She explained that elevated heart rates often coincide with blood loss, and she thought it was best for us to proceed to the ER. Fear of the unknown and lack of information began to take hold once again. As I waited for the nurse to bring the paperwork for the ER, it dawned on me that this was the first time either of my kids was ever going to the ER.
After a short wait, the nurse practitioner, not the nurse, returned with the paperwork. She sat next to me on the bench and gave me a hug. She said, “I wanted to tell you that I have been a nurse practitioner for almost 30 years, and I have seen everything, believe me. I just want you to know in case no one has told you that you are an incredible mom. I see you with your daughter, and I see it. Know you are doing everything you can for her, and I know it isn’t easy.” It was the kindest thing she could have said to me and strengthened me for the next leg of the journey. I barely held it together as I left the office. I cried all the way home.
Todd arrived at the house at the same time as Emily and me. We gave Emily a few minutes to rest and regroup before heading to the ER. We made sure she was dry and comfortable and let her crawl around for a bit. We turned on The Wiggles, and she was content to have a break. Todd and I loaded Emily and the additional gear into the van. Off to the ER, we went.
When we got to the security gate at the ER, the security guard informed us only one of us could go in. I tried to reason with him that Emily would need both of us for this visit, but he told me it was policy. Todd asked him to get a supervisor, and he refused, so Todd pushed Emily past him and went into the ER. This was great, except I was outside with all the paperwork and insurance information, and the security guard was not letting me pass. I was crying (again) and told him I had all of my daughter’s medical information. He states, quite rudely, that my husband made the decision as to who was going in, and it wasn’t me. I was trying to remain calm as I was wearing my blue Pause Breathe Reflect shirt (and the hoodie too). A moment later a nurse came outside and escorted me into the building. The security guard made some other comment under his breath, but I just walked past him and ignored it.
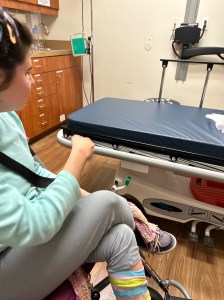
Things went better than expected inside. The ER was bursting at the seams with patients. We huddled into a corner, and staff came to check us in. We went to another corner of the ER where our nurse (the same nurse that freed me from security), Heather, began to take Emily’s vitals. She prompted Todd and me where to hold Emily’s arm and shoulder to reduce motion. She was kind and patient. She noted that Emily’s heart rate was elevated, and it was probably because she was pissed off that she kept trying to get her blood pressure, and she was uncomfortable. After a few adjustments, she got Emily’s blood pressure! I was thrilled and may have told her she had to go with us to every future medical appointment with our family. Her kindness and tolerance of Emily were above and beyond. As we discussed medications and history, she shared she has two adult sons with Autism. Oh, we were in the hands of someone who “gets it”.
The lab tech, Justin, came into the waiting area to draw blood and had zero issues. I think all the commotion in the waiting room and activity distracted Emily. She was in her wheelchair with Mom and Dad by her side, and the blood pressure cuff was out of sight. She barely made a peep, and her squirming was easy to minimize.
The doctor did another exam. My poor girl. She could not find any obvious issues. Emily’s labs looked good. She prescribed some steroid suppositories (oh joy) for the next 10 days and told us to follow up with the GI specialist for further diagnostic testing.
I dropped Emily and Todd off at the house and went to pick up the prescription that was not covered by insurance (even though it is generic and there is NO alternative). It was almost 9 pm, and I was just done. I handed the pharmacist my debit card with gratitude that we had the money to cover the cost.
For now, we treat the symptom and wait for answers. It is difficult to watch your child face a health issue and not be able to express what she is feeling. Is she in pain? We were asked that question many times today, and we cannot really answer the question, and that part sucks. I am grateful we have access to medical care, even if the system is screwed up. I am thankful that Todd was there to support me. I grieve because Emily is unable to communicate her pain and discomfort. I am grateful for Nurse Heather. I am disappointed that Emily’s medical care is not as good as it was when she was a child. I am grateful Emily has the support of a family that loves her and wants the best for her. I reside in grief and gratitude as I reflect on the past 24 hours.

God Bless you Billie ❤️❤️❤️
LikeLiked by 1 person
Thanks for the love and support Patti.
LikeLike